A dry mouth is not good for oral health, as saliva helps to chew the food better and control the cavity development on teeth. It would be interesting to look at dry mouth causes and remedies. Common causes for dry mouth are medicine side-effects, disease, dehydration, etc. While there are some remedies for it like preventing tooth decay, fluoride treatment, and good oral hygiene.
Xerostomia, is the condition of not having enough saliva, or spit, to keep the mouth wet. Dry mouth can happen to anyone occasionally—for example, when nervous or stressed. However, when dry mouth persists, it can make chewing, eating, swallowing, and even talking difficult.
Xerostomia, more commonly known as dry mouth, is not a disease in itself. Rather, it is a symptom of many other diseases and conditions. These conditions cause saliva production to decrease or stop.
Saliva moistens your mouth and helps you to swallow and taste food. It helps in fighting cavities by washing away food and plaque from the teeth. It also helps to neutralize acids in the mouth that harm tooth enamel.
If you have less saliva in your mouth, your teeth and gums are at increased risk of tooth decay. People with xerostomia also are more likely to get illnesses that affect the soft tissues of the mouth, such as yeast infections (thrush).
In addition, your diet may be affected because you cannot taste food as you normally would. People with complete dentures who develop xerostomia also may notice that their dentures lose some of their suction. They may feel loose.
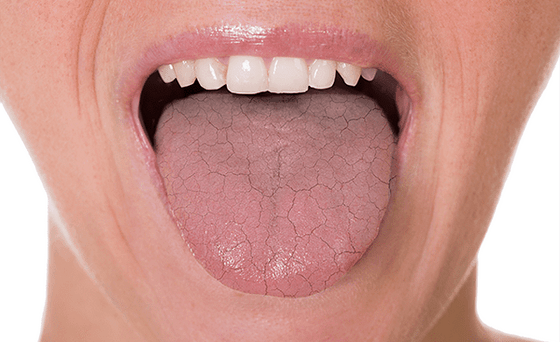
Xerostomia may occur for several reasons. It is because the salivary gland does not work properly. Some common causes include:
- A side effect of medicine : Hundreds of drugs can cause dry mouth. These include pain relievers and medicines for depression, cold symptoms, muscle spasms and allergies.
- Medicines are the most common cause of xerostomia. Older people often take many medicines, including those most likely to cause dry mouth. Medicines for diabetes, parkinsons disease and sjogrens syndrome are common causes for this condition.
- A complication of diseases and infections: Dry mouth occurs more often among people with certain diseases. They include diabetes, anemia, cystic fibrosis, rheumatoid arthritis, high blood pressure and HIV infection. Xerostomia also occurs with Sjögren’s syndrome. In this disease, the body’s antibodies attack the salivary and tear glands. Some viral infections, such as mumps, also affect saliva production and cause xerostomia.
- Dehydration: Any condition that leads to loss of body fluids can also cause xerostomia. These conditions include fever, excessive sweating, vomiting, diarrhea, blood loss or loss of water through the skin after a burn.
- Radiation therapy : Xerostomia is a common side effect of radiation therapy to treat cancers in the head and neck.
- Surgical removal of the salivary glands: If a mass develops in a salivary gland, surgical removal of the gland may be recommended.
Symptoms
Although xerostomia is a symptom, it often occurs along with other symptoms. These may include:
- Frequent thirst
- Burning or tingling sensation, especially on the tongue
- Red, raw tongue
- Sores in mouth or at corners of lips
- Difficulty swallowing
- Problems with taste
- Sore throat and hoarseness
- Bad breath
- Problems with speech
- Dry nasal passages
- Dry, cracked lips
- Increase in dental problems, such as cavities and periodontal disease
- Difficulty wearing dentures
- Repeated yeast infections in the mouth
Diagnosis
Xerostomia is a symptom, not a disease. Tell your dentist and hygienist about your dry mouth. They will try to determine the cause. Your dentist will ask you about your medical history and your symptoms. He or she will ask about any drugs you are taking. This includes prescription, nonprescription and herbal remedies. The dentist also will examine your mouth.
He or she will assess the flow of saliva and look for cracks, sores, and signs of cavities and gum disease.
Prevention
Xerostomia is a condition where the mouth becomes dry due to a decrease in saliva production. It is important for xerostomia prevention, as saliva is essential for chewing food and keeping it cavity-free. Some of the ways to prevent Xerostomia are controlling tooth decay, fluoride treatment, chewing sugarless chewing gums, dental treatment, and keeping up good oral hygiene.
To prevent dry mouth, avoid things that cause it, if possible. For example, if dry mouth is related to a medicine, your physician may be able to prescribe a drug that causes less dryness. Do not overuse cold medicines and antihistamines. You also can take steps to prevent or manage the symptoms of dry mouth.
Treatment
The treatment of xerostomia focuses on three areas:
- Relieving symptoms
- Preventing tooth decay
- Increasing the flow of saliva, if possible
- Your doctor will recommend that you practice good dental hygiene. This means that you should brush and floss properly. You also should have regular dental visits. In the office, your dentist or hygienist also will regularly apply fluoride to your teeth. You may be given a prescription for a fluoride rinse to use at home. Your physician may work with your dentist to manage your condition.
- Treatment is based on how severe your problem is and what caused it. Fluoride treatments can be prescribed to help prevent cavities. Artificial saliva is available over the counter as a rinse, spray or gel. Depending on your medical condition and diagnosis, a physician or dentist may prescribe a drug that causes more saliva to be released.
To relieve your symptoms, try the following:
- Drink water often to keep your mouth moist. Carry water with you. Sip it throughout the day. Keep water by your bed at night.
- Suck on sugar-free hard candies, ice chips or sugar-free ice pops.
- If you chew gum, try sugarless gum.
- Use an over-the-counter oral moisturizer or saliva substitute.
- Use mouth rinses or mouthwashes that do not contain alcohol.
- Avoid salty foods, dry foods (crackers, cookies, toast) and foods and beverages with high sugar contents.
- Avoid drinks containing alcohol or caffeine. These increase water loss by triggering frequent urination.
- Avoid smoking.
- To reduce irritation of dry tissues, use a moisturizer on your lips and a soft-bristled toothbrush on your teeth and gums.





